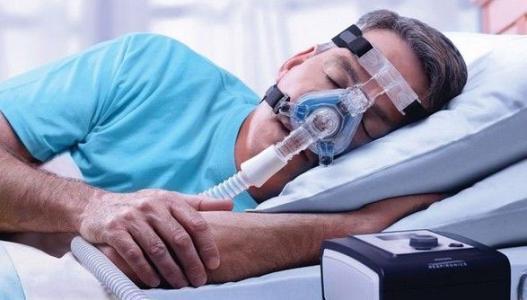
Pathophysiological characteristics of chronic obstructive pulmonary disease:
(1) Small bronchial inflammation, increased mucus in the wall. General anesthesia should avoid the use of inhalation anesthetics to stimulate respiratory secretion, and at any time to clear the tracheal secretions.
(2) Small airway resistance increases, resulting in obstructive ventilatory dysfunction. Ventilation and forced vital capacity (FVC) decreased significantly.
(3) Recurrent episodes of bronchial inflammation can lead to pulmonary fibrosis and pulmonary stenosis or occlusion of the pulmonary capillaries. The result is pulmonary arterial hypertension, and severe cases can develop pulmonary heart disease. Therefore, the patient's cardiopulmonary compensatory function is poor. Can not tolerate hypoxia, blood loss, infusion overdose and anesthesia too deep
(4) Inflammation of the lungs, increased oxygen uptake in the body, intrapulmonary shunting and pulmonary shunt (indicated by increased broncho-pulmonary circulation due to pneumonia), and limited diffusion of alveolar-end capillaries, these are sufficient to cause varying degrees of low Oxygenemia, so oxygen therapy must be strengthened during and after anesthesia.
1, chronic bronchitis
A history of chronic non-specific inflammation of the bronchus for more than two years, often coughing, coughing, and even asthma. Due to congestion and edema of the bronchial mucosa, thickening of the wall of the tube and narrowing of the wall of the tube, obstructive ventilatory dysfunction occurs.
2, emphysema
Emphysema is the most common complication of bronchial disease.
3, bronchial asthma
Allergic diseases are induced by certain allergens such as infections, physical and chemical stimuli, drugs or immune stress.
4, bronchiectasis
The bronchial wall is damaged due to inflammatory changes caused by smooth muscle and elastic fibers. When the thoracic cavity is inhaled, the bronchus expands due to the action of pulling outwards. When the breath is lost due to elasticity, it cannot be retracted, ie, bronchiectasis is formed. .
5, silicosis
Long-term inhalation of silica dust in the air causes silicosis, formation of orbital nodules in the lung parenchyma, and subsequent development of extensive pulmonary fibrosis, reduction of the pulmonary capillary bed, increased resistance to pulmonary circulation, paralysis of pulmonary nodules and compression of lung tissue and bronchioles. Obstruction, which can be a sign of severe emphysema, eventually causing severe ventilation and ventilation dysfunction.

Anesthesia treatment

(I) Estimate before anesthesia
1, medical history and physical examination
2, laboratory testing
3, the estimation of respiratory function
(B) Preparation before anesthesia and preoperative medication
The purpose of preparation before anesthesia is to improve respiratory function and improve cardiopulmonary compensatory ability. Increase patient tolerance for surgery and anesthesia. The focus of preparation is to control respiratory infections, relieve bronchial spasm, and perform breathing exercises, but this should generally be done during remission of lung disease.
1, regular preparation
Instruct patients to perform breathing exercises. When chest breathing is no longer effective in increasing pulmonary ventilation, deep and slow urethral breathing should be practiced to increase the diaphragm's range of motion.
For more pleural effusion, suction flow should be taken before surgery to improve ventilation. Inhalation of N2O during closed pneumothorax may increase the degree of pneumothorax, it should be avoided. Persons suffering from closed pneumothorax should be punctured by a thoracic gas to promote lung expansion. Patients with hypoxemia should be treated with oxygen before surgery in order to increase blood oxygen pressure before surgery.
For those who have a long history of smoking, smoking should be prohibited for at least two weeks before surgery. Although the concentration of carbon monoxide and hemoglobin may decrease after 12 hours of smoking, bronchial secretions and ventilation need to be banned for at least two weeks to improve.
2, control respiratory infections
Acute respiratory infections are generally contraindicated unless emergency surgery is performed. With bronchiectasis should be controlled by inflammation, two weeks after the reduction in sputum and then surgery to safety. Recent hemoptysis should be regarded as a relative contraindication for surgery. Chronic respiratory diseases are routinely administered with antibiotics 3 days before surgery to prevent lung infections.
3, relieve bronchial spasm
Chronic bronchitis with asthma attack, suggesting the presence of bronchial spasm, in addition to the use of antibiotics to control infection, but also use β2 receptor stimulants for aerosol inhalation, such as salbutamol, each dose of 100 ~ 200ug, there is a clear connection to the bronchial smooth muscle Sputum effect, resulting in expansion of the bronchus, reducing airway resistance and drainage of sputum efficacy, the side effects on the heart is very small.
4. Treatment
Chronic respiratory diseases often result in abnormally thick and thick small airway secretions. Physical therapy is performed before surgery. For example, patting the chest and back can help relieve sputum; patients can be encouraged to cough and keep the airway open; people with more sputum can be used for position. drainage. Sticky people can take the following two types of tincture:
4.1 Diluted drugs such as ammonium chloride 0.3 ~ 0.6g, oral 3 times a day; bromamine hydrochloride 8 ~ 16mg, 3 times a day orally; ipecac syrup 0.5 ~ 1.5ml, 3 times a day, have stimulated bronchial Secretion to dilute the role of sputum
4.2 Sputum solution depolymerization drugs such as acetylcysteine, with its 5% ~ 10% aqueous solution and then add prion protein decomposition, fracture, so that the viscosity of phlegm fluid drop, easy to cough. Appropriate intravenous fluids also have the effect of diluting phlegm and making it easier to cough up.
5, medication before anesthesia
Opioids can significantly inhibit the respiratory center and should be used as an anesthetic medication. Although morphine has a strong analgesic effect, it has the side effect of excitatory vagal nerve release of histamine and asthma, and the duration of the effect is too long, can also weaken the cough reflex, so it is unfavorable for postoperative drainage. Pethidine can relax bronchial smooth muscle; fentanyl has anti-histamine and anti-5-hydroxytryptamine effects, which can relieve bronchial spasm. Promethazine is an ideal premedication drug. It has strong sedative and antihistamine effects and should be combined with pethidine. Adults commonly use promethazine 25mg and pethidine 50mg intramuscularly.
Anesthetic choice
Anesthesia choice should be combined with the characteristics of patients with respiratory insufficiency. The ideal anesthetic methods and drug selection principles are:
1, less interference in the respiratory circulatory system;
2, sedation, analgesia and muscle relaxant effect;
3, poor surgical reflex inhibition;
4, recovery after surgery quickly;
5, fewer complications.
The choice of anesthesia method
1. Local and nerve block have little effect on respiratory function, retain spontaneous breathing, and can actively cough up tracheal secretions. Therefore, it is safer for patients with respiratory diseases, but there must be limitations in use. Nerve block is only applicable to Neck and limb surgery; local anesthesia has insufficient pain, muscle weakness is not satisfied with the weaknesses, it is only suitable for short surgery.
2, spinal anesthesia analgesic and muscle relaxation effect is good, often applies to the abdomen, pelvic and lower limb surgery. Spinal anesthesia interferes more with the circulatory system and is less preferred. Epidural block of the chest or upper abdomen can significantly reduce the ventilatory reserve function due to the simultaneous obstruction of the respiratory muscles. Therefore, it is not suitable for patients with severe respiratory dysfunction.
3, endotracheal anesthesia for patients with severe illness, poor respiratory function or hypoxemia patients, also applies to patients with complex surgery, long time, tracheal intubation can reduce respiratory ineffective cavity, adequate oxygen supply and conducive to respiratory management, also Respiratory secretions can be removed at any time as needed.
Anesthetic treatment
About 13% to 25% of postoperative deaths in coexisting respiratory diseases died of pulmonary complications. Proper postoperative treatment is of great significance in preventing complications and reducing operative mortality. After anesthesia, emphasis should be placed on encouraging coughing, maintaining airway patency, maintaining a stable circulation, using antibiotics to prevent lung infections, and correcting water-electrolyte disorders and acid-base imbalances. These are all extremely important prevention principles. In addition, patients with thoracic surgery should pay particular attention to the following aspects:
1, the maintenance of respiratory function
2, wound pain treatment
3, clear respiratory secretions
4, oxygen therapy